According to a McKinsey survey, seniors are extremely loyal. The survey found 81% of Medicare customers 75 or older said they renewed their plans without shopping for a new one. 76% of 71 to 74-year-olds and 70% of 65 to 69-year-olds reported the same. For marketers selling Medicare Advantage plans, that loyalty can lead to the lifetime value of Medicare Advantage members outpacing individual or group plan members.
As a result, marketing Medicare Advantage plans can generate significant ROI for insurers. Here are some tips when marketing Medicare Advantage plans:
Create a Competitive Product
That same McKinsey survey referenced earlier also noted an interesting result: Price or total cost isn’t the determining factor when choosing a Medicare Advantage plan. Members value having their doctor and/or hospital in-network; it ranked as one of the top three factors when selecting a plan. A choice among doctors and hospitals also plays a significant role in choosing a plan. Finally, consumers value an insurer’s brand and reputation when making a purchasing decision, which we’ll discuss a bit later.
Successful marketing starts with desirable products and Medicare Advantage plans are no different. Creating a Medicare Advantage plan requires significant research and product strategy development to effectively create competitive products. Entering the Medicare Advantage market can be a costly undertaking. Failing to create a realistic strategic plan and product roadmap in what is usually a competitive market anchored by the largest health insurers in the US may lead to less than favorable results.
How does an insurer enter the Medicare Advantage market? That depends on a lot of factors, including the insurers’ existing book of business. For example, an insurer with a strong commercial footprint can leverage that footprint to market to age-in populations, those that are or will be turning 65. Those with a strong Medicare supplement member count can try to convert those members to Medicare Advantage plans.
All insurers have strengths and weaknesses. Identifying your strengths and discovering how they’ll play in the Medicare Advantage market can deliver easy wins and momentum.
Follow the Rules
To prevent Medicare Advantage plans from providing misleading or even fraudulent information about a plan’s costs or benefits, the Center for Medicare and Medicaid Services (CMS) has published a set of regulations those marketing Medicare Advantage plans must follow. The regulations define what constitutes marketing activities and then define rules for various activities. Among the topics covered:
- General communication requirements around anti-discrimination, referring to plans by standardized names, hours of operation requirements, prohibited terminology and statements, product endorsements and testimonials, and more.
- General marketing requirements like plan comparisons, marketing through unsolicited contacts, telemarketing, gifts, marketing star ratings, open enrollment period marketing, and reward and incentive programs.
- Outreach activities like educational events, marketing/sales events, and individual marketing appointments
- Marketing within a healthcare setting, like provider activities.
- Marketing on websites and social/electronic media including required website documents, general website requirements, social media regulations, and mobile applications.
- Call centers, including representative requirements and standards, hours of operation, scripts, telesales and enrollment scripts, and other call center guidance
- Agent/Broker activities, oversight and compensation requirements
- The use of Medicare beneficiary information obtained from CMS
To avoid penalties, you must understand and apply CMS’ Medicare marketing guidance when developing a marketing plan and materials. Be sure to include a compliance review in every marketing plan.
You can find the complete CMS Medicare Advantage marketing guidance here.
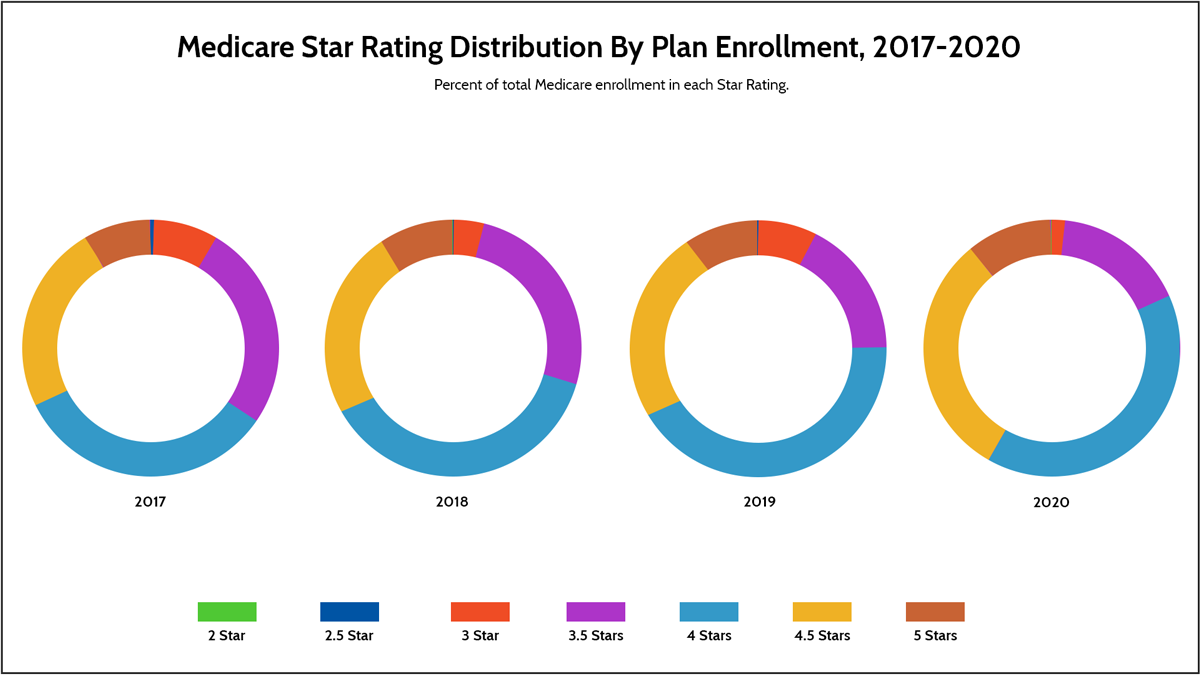
Have a Star Rating Optimization Plan
CMS created a Medicare star rating system to help beneficiaries compare plan performance and quality. The five-point scale measures:
- Access to preventive services to keep members healthy
- Management of chronic conditions
- The member experience
- Member complaints
- Call center customer service
Medicare prescription drug plans have similar measurements to determine star ratings.
Product reviews have a significant impact on product sales. The Medicare Advantage market is no different. An analysis by Navigant, for example, found that for plans with a 3 star or less rating, just a 1-star increase could lead to an 8 to 12 percent increase in enrollment.
As a result, your organization must create a plan to optimize star ratings. Read our guide to Medicare Star Ratings for tips regarding how to improve your star rating.
Understand Enrollment Periods
Medicare Advantage has some enrollment periods to keep in mind when developing your marketing plan. Here’s an overview of the enrollment process:
- The initial enrollment period (IEP) occurs throughout the year and is based on a potential member’s birthday. Members can enroll in Medicare from three months before their 65th birth to three months after their 65th birthday.
- The annual enrollment period (AEP) occurs from mid-October to early December every year. During this period, members can join, switch or drop a plan.
- The Medicare Advantage Open Enrollment period occurs from Jan. 1 to March 31 each year. Individuals enrolled in a Medicare Advantage Plan can switch to a different Medicare Advantage plan or original Medicare once in this period.
These dates matter because they give timelines when your marketing will have the most impact. A best practice would dictate that you create segments and marketing plans for each enrollment type based on data that you have. For example, if you have existing group or individual customers who will be turning 65, create a direct mail campaign around their birthdate.
CMS prohibits knowingly marketing during the Medicare Advantage Open Enrollment period (Jan. through March). You can still market to age-ins that fall in this period. However, you are prohibited from specifically and knowingly targeting those who have enrolled. CMS also doesn’t allow marketing for an upcoming plan year’s AEP before Oct. 1.
Start with a Marketing Plan
Next, it’s time to create a marketing plan. Here are some tips:
SWOT and Competitor Analysis
If you haven’t done a SWOT and competitive analysis, that’s good background data to have to better understand your Medicare strengths, weaknesses, opportunities, and threats. Understanding your competition can also help with messaging. For example, if you’ve got a superior network, highlight your network size in your marketing mix.
Define Your Audience
You must understand your audience’s motivations, their buying journey, and who they are so that you can create the most impactful marketing campaign. Some things to consider:
- Demographics — Things like the audience’s age, location, income, marital status, how many children they have, etc. can help you better understand your potential buyers and craft more effective messages as well as determine specific tactics.
- Health Care Goals and Motivations — What do consumers want from their Medicare Advantage plan? For example, you may find that your audience has a hard time navigating the health care system. They want a plan that is more personalized and helps them understand where and how to get care.
- Technology Aptitude — If your target audience has poor technology skills and needs help doing simple things like navigating a website, you don’t want any processes that are overly reliant on navigating an overly complicated site.
- Social Media Use and/or Media Consumption Habits — Knowing where your target audience congregates can help you target specific tactics to that audience. For example, if most of your audience is active for hours a day on Facebook, it makes sense to invest in targeted Facebook ads. If a majority of your audience reads Modern Gardener, invest in an ad there. If they use public transportation, invest in bus stop advertising.
Understanding your audience is the key to maximizing your marketing investment.
Start with the end in Mind
Your marketing plan should start with the end in mind: What are you hoping to accomplish? Do you want to achieve a specific retention rate during AEP? Need to add X members during this calendar year’s IEP? Do you want more market share?
Defining your goals before you consider tactics will improve the execution of your marketing plan. It forces you to focus on what you wish to accomplish. That focus enables you to make better choices based on what metrics you want to improve.
Get Tactical
With audiences defined and goals identified, it’s time to start determining tactics you’ll use to market to your target audiences. Some tips:
- Take an omnichannel approach. In the past, insurers enrolling seniors in Medicare plans have largely focused on tactics like direct mail and in-person events and meetings. But today’s seniors are more tech-savvy and active online, especially those enrolling in Medicare for the first time at age 65. Taking a more omnichannel approach can prove cost-effective. Channels/tactics to incorporate in your marketing mix include pay-per-click on keywords frequently searched by your target audiences. Retargeting to individuals who have visited your Medicare Advantage landing pages can help your brand follow them around the Internet after they leave, keeping you top of mind. Digital video advertising on YouTube is also an option. Baby boomers tend to be active on the streaming video site.
- Make sure events and in-person meetings follow CMS guidelines. We discussed CMS guidelines earlier, but it’s important to reiterate: If you are hosting events or in-person meetings there are guidelines you need to follow to maintain compliance. For example, educational events can’t include a marketing component, meaning you’re not allowed to distribute marketing materials or enrollment forms after the event. Individual marketing appointments must only concern previously agreed-upon plan products and can’t solicit enrollment applications for a Jan. 1 effective date until Oct. 15.
- Don’t Forget About Retention — Retaining your existing Medicare Advantage members should be part of your marketing plan. In addition to focusing on the member experiences that matter the most based on your internal data, always be testing new approaches to engaging your members. Whether it’s creating a small test of a new communication tactic or message or leveraging member survey results to improve your messaging, always be on the lookout for ways to improve your member retention efforts. It’s also important to understand what makes members leave — and how to identify members at risk. Whether that’s tracking whose premiums are increasing or whose networks have changed or who’s left negative feedback about interactions with customer service, leverage your data to understand who is most at risk and create communication strategies that mitigate that risk.
- Be Helpful — Finally, be helpful. In today’s business climate, insurers that focus on helping members and buyers make informed decisions are ultimately the insurers that will earn buyer and member trust. Deceptive tactics may result in short-term games, but almost always end in long-term brand damage. For example, Humana has educational content detailing tips for choosing the right Medicare coverage while Cigna has a good explainer of Medicare Advantage plans. Whatever marketing tactics you provide, remember to also have a mix of educational content available to help consumers make the best choice they can.
Certifi’s health insurance premium billing and payment solutions help healthcare payers improve member satisfaction while reducing administrative costs.